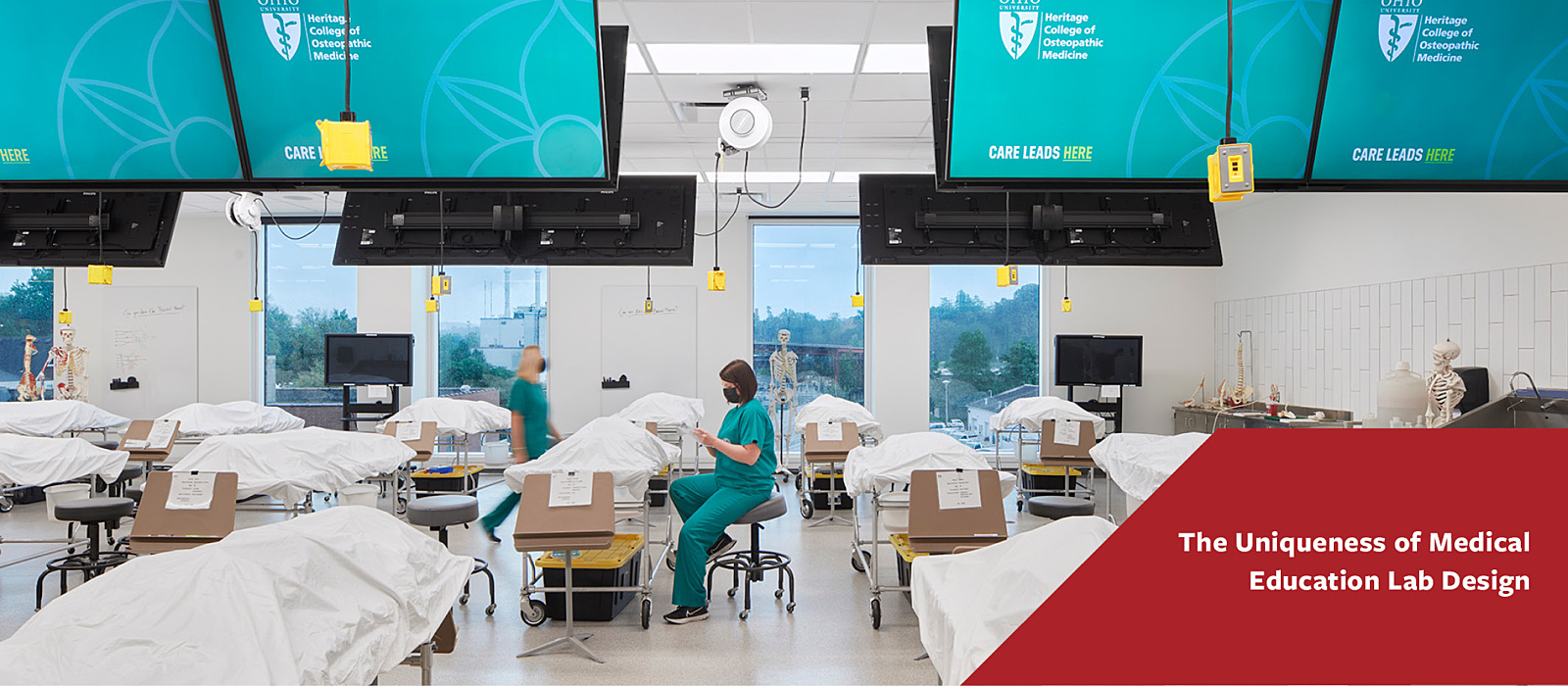

Nurturing Tomorrow’s Healers
Rocco Gallo
and
Evan Hammersmith
and
Kris Peterson
and
Natasa Kuljanin
Oct 13, 2023
In the landscape of higher education, medical education distinguishes itself with one of the most exacting and challenging curricula. Delve into three key strategies that highlight the prioritization of student well-being in the design of medical education facilities.
Charting the Course to Achieve Campus Carbon Emissions Goals
Joe Hofstetter
Jul 24, 2023
Infrastructure Required for Electric Vehicle Charging Stations
James T. Cicero
Jul 20, 2023
More than 2 million EVs are now on the road in the U.S. As the number of electric vehicles on the roads continues to grow, a question arises: Is the electrical infrastructure of public buildings, apartment complexes, and workplaces prepared to handle the increased load of electric vehicle charging stations?
Creating Smart Buildings for Better Experiences and ROI
Joe Hofstetter
and
Brian Tenney
Aug 26, 2022
How a smart building can deliver payback through improved efficiency and ease of use
Energy Savings Is More than MEP
Mattias DeDoes
and
Joe Hofstetter
Mar 22, 2022
Energy savings are often equated with MEP improvements and not much else. But when we limit the search for energy savings to MEP systems, we leave opportunities for savings on the table. Here’s an overview of how to find more savings and improve your environmental impact.
3 Key Concepts for Code-Compliant Outpatient Healthcare Facility Design
Dave Curfman
Feb 01, 2022
What Design Teams Need to Look for and Why Your MEP Engineer (Should) Ask So Many Questions
Taking Prefab to the Next Level with Industrialized Construction
Rocco Gallo
and
Matthew Morgan
Nov 29, 2021
What if architects and engineers worked prefabrication directly into their designs?
Post-Pandemic, 2 Big Ways to Change Healthcare Design for the Better
James T. Cicero
and
Rocco Gallo
Nov 18, 2021
Two recommendations for design teams and healthcare organizations to apply today
FGI Guidelines: What’s New for 2022
Rocco Gallo
Nov 15, 2021
5 noteworthy changes coming to the 2022 FGI Guidelines, from the 2021 Healthcare Design Conference
Smart from the Start: Keys to a Successful Building Integration Project
Brian Tenney
Aug 13, 2021
With the amazing potential that building integration offers, how do you make it work for your facility?